ROSA Robotic Technology for Minimally Invasive Brain Surgery
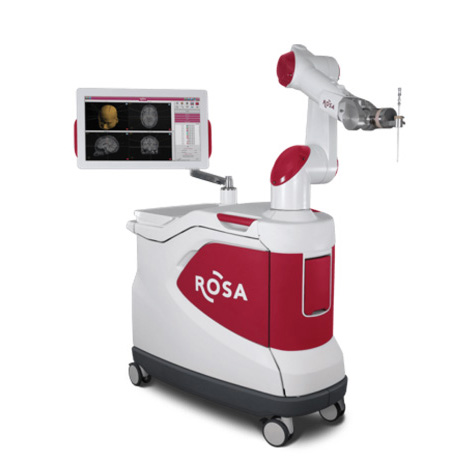
ROSA ONE Brain is a surgical navigation and positioning system using robotic technology that allows surgeons to place instruments in the brain through tiny holes in the skull.
Conventional brain surgery requires a craniotomy, which is the surgical removal of part of the bone from the skull to expose the brain. This common surgery is highly invasive and can lead to long recovery times. Affectionately known here as the “ROSA robot,” ROSA ONE Brain allows many neurosurgical procedures to be performed in a minimally invasive way for neurological conditions such as epilepsy and seizures, Parkinson’s disease or brain tumors.
The ROSA Robot in Action
ROSA ONE Brain can be used in variety of procedures to explore and treat disorders of the neurological system and the brain. These include:
- Deep brain stimulation (DBS). A device delivers electrical pulses to brain cells for the treatment of movement disorders.
- Stereo-electroencephalography (SEEG). Used in epilepsy patients to determine the seizure focus, or the “source” of the seizures.
- Stereotactic biopsy. Using guided instruments to locate and remove a sample of some tissue from a living body to discover the presence, cause or extent of a disease.
- Ventricular endoscopy. The use of an endoscope to perform surgery within the fluid-filled spaces of the brain, also called the ventricles.
- Transnasal endoscopy - an endoscopic method which is performed by the nasal route using a thin endoscope. This is generally used to allow minimally invasive access to the pituitary gland and skull base.
Epilepsy is a neurological disorder marked by sudden recurrent episodes of sensory disturbance, loss of consciousness, or convulsions, associated with abnormal electrical activity in the brain. It is highly prevalent, highly disruptive to daily life, and highly undertreated due to stigma and lack of education of current treatment options (among both patients and physicians).
According to the U.S. Centers for Disease Control and Prevention, in America there are 3.4 million people that currently either take medication to try to control seizures, or have had a seizure in the past year. Around 56 percent of epilepsy patients have seizures that are not controlled by medication. This is called refractory epilepsy, which is also known as intractable or drug-resistant epilepsy.
Mapping the Brain and Honing in on Targets
A neurosurgeon uses ROSA and its planning software to create a 3D map of the patient’s brain and plan out exact pathways needed to carry out the procedure.
ROSA ONE Brain follows the paths outlined by the surgical plan, and the surgeon carries out the surgery using the robot as a guide to reach a deep brain target for the placement of surgical instruments.
Benefits of Robotic Surgery with ROSA Brain
Minimally invasive surgery using ROSA may allow surgeons to achieve shorter operating times and eliminate the need for traditional craniotomies. Generally, patients undergoing a robotic surgery procedure experience significantly less pain, less loss of blood, fewer side effects, less scarring, shorter recovery period and a faster return to normal activities.
Contact Us
At RWJBarnabas Health, our highly skilled neurosurgeons are leading the way in implementing ever-advancing medical treatments to serve our patients better. To learn more about the ROSA ONE Brain system at RWJBarnabas Health, request an appointment with one of our neurosurgery specialists today.
